Managing All GLP-1 Side Effects: Complete Guide
- January 15, 2026
- 0
Side effects are common during GLP-1 treatment, especially in the first few weeks. This complete guide explains what’s normal and when to get help.
Side effects are common during GLP-1 treatment, especially in the first few weeks. This complete guide explains what’s normal and when to get help.

Managing GLP-1 side effects requires a combination of immediate relief strategies and long-term prevention habits tailored to your specific symptoms. Most side effects peak during the first 2-4 weeks and improve significantly as your body adjusts to medications like Ozempic, Wegovy, or Mounjaro.
Key side effects and management approach:
This comprehensive guide provides practical, actionable solutions for common GLP-1 side effects, plus critical information on when symptoms require medical attention versus home management.
Table of Contents
Toggle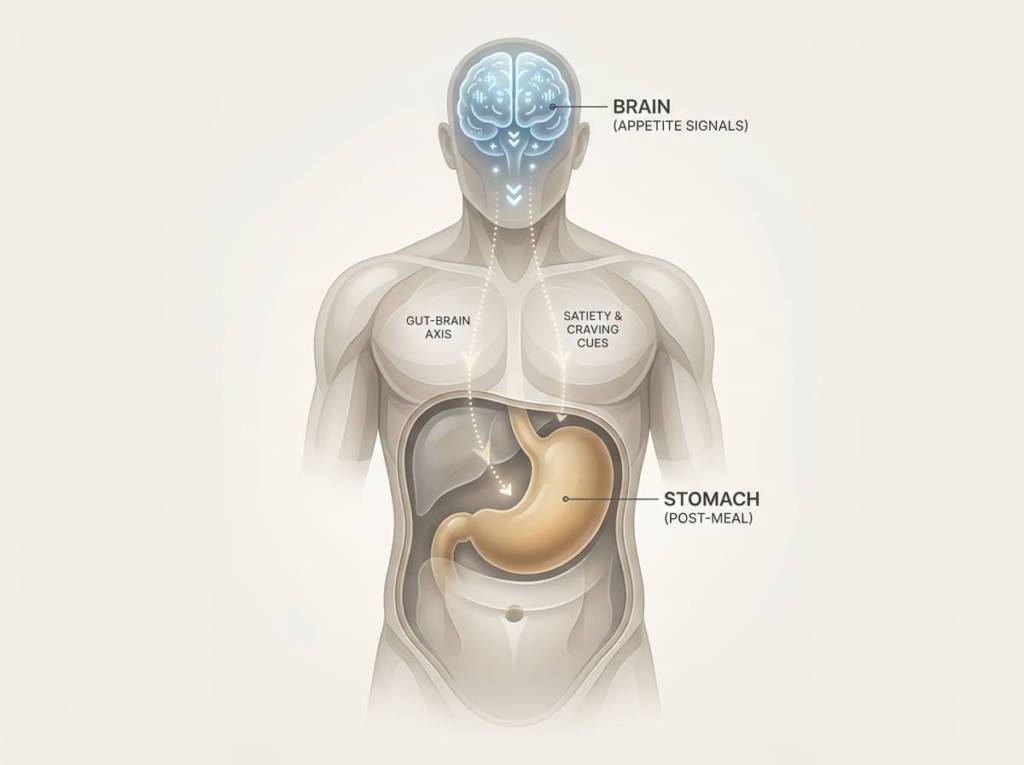
GLP-1 medications slow down how quickly food leaves your stomach and change the hunger signals in your brain. That’s exactly how they help you lose weight. But these same mechanisms create side effects that most people experience at some level.
Here’s what commonly happens:
How bad these side effects feel varies wildly from person to person. Some people breeze through with barely any discomfort while others struggle more during those first few weeks. You might feel them intensely or not feel anything at all.
The good news is most side effects peak in the first 2-4 weeks and then start getting better as your body adjusts.

GLP-1 nausea is hands down the most common complaint with weight loss medications. It usually kicks in within 24-72 hours of your first shot and thankfully gets much better after 2-4 weeks.
Here’s what actually helps:
Want more help? Check out our full guides on 10 Best Foods to Eat for GLP-1 Nausea and How to Stop Nausea on GLP-1: 12 Relief Tips That Work.

Constipation happens because GLP-1s slow everything down in your digestive tract, not just your stomach. This is one of those side effects that tends to stick around longer and needs ongoing attention.
Here’s your action plan:
Need more details? We’ve got you covered in GLP-1 Constipation Relief: What Actually Helps and High-Fiber Foods for GLP-1: Beat Constipation.

Constipation gets more attention, but some people get hit with diarrhea instead. This especially happens during the first few weeks or when you bump up your dose. Sometimes it even alternates with constipation, which is super frustrating.
Quick fixes that work:
When to call the doctor: If you’re running to the bathroom more than 6 times a day, it lasts more than 2-3 days, or you see blood or have a fever, call your doctor.

Some people get acid reflux for the first time on GLP-1s, or it gets worse if they already had it. When your stomach empties slower, acid has more opportunities to creep up into your throat, especially when you lie down. Some research shows a link between acid reflex and short-acting form GLP-1 medication.
What actually helps:
Important: If you get severe heartburn, trouble swallowing, or chest pain, get it checked out. Don’t mess around with those symptoms.

Feeling wiped out is super common during your first few weeks. You’re eating way less than usual, you might not be getting all your nutrients, and your body is adjusting to how the medication affects your blood sugar and metabolism.
Energy boosters that work:
When to worry: If you can barely get through your day, you’re still exhausted after 4-6 weeks, or you’re dizzy and your heart is racing, talk to your doctor.

Reduced appetite is literally the point of GLP-1 medications. That’s how they help you lose weight. But sometimes your appetite gets so suppressed that you struggle to eat enough to stay healthy.
How to eat when you’re not hungry:
Keep in mind: Reduced appetite helps you lose weight, but you still need to feed your body. If you’re consistently eating under 1,000 calories or you can barely eat anything, talk to your doctor about adjusting your dose or working with a nutritionist.
Beyond tackling individual symptoms, these overall strategies help you prevent or minimize side effects from the start.
Follow the slow titration schedule. Don’t rush to increase your dose, even if you think you can handle it. Those gradual increases give your body time to adjust. Jumping up too fast almost always backfires with worse side effects.
Slow way down when you eat. Take at least 20-30 minutes to finish a small meal. Put your fork down between bites. Chew each bite until it’s basically liquid. This takes pressure off your already-slow digestive system and helps you notice when you’re full before you overdo it.
Make water a non-negotiable habit. Drink water consistently all day long. Get most of your fluids between meals instead of with meals so you don’t overfill your stomach. Good hydration prevents or reduces a bunch of different side effects including nausea, constipation, and fatigue.
Experiment with injection timing. A lot of people inject at night so the worst nausea happens while they’re sleeping. Others prefer mornings. Try different times to see what works best for your body and schedule.
Stay away from problem foods. Greasy, fried, spicy, and heavily seasoned foods make side effects worse for most people. Strong-smelling foods can trigger instant nausea. Really rich or heavy foods sit like a rock in your slow stomach. Stick with simple, mild foods, at least while you’re adjusting.
Keep moving regularly. Daily gentle movement helps your digestion, energy, and overall wellbeing. Walking is perfect. Even 15-20 minutes makes a difference. Try to move after meals when you can.
Track what’s happening. Write down what you eat, when symptoms hit, and what helps. Over a few weeks, you’ll start seeing patterns that help you figure out what your body needs and what to avoid.
Build a routine. Eat around the same times each day. Drink water consistently. Keep a regular sleep schedule. Move your body daily. Routine helps your body adjust way more smoothly.

Most GLP-1 side effects you can handle at home. But some symptoms mean you need medical help right away. Here’s how to know the difference.
Call 911 or go to the ER for:
Severe, non-stop vomiting: If you’re throwing up multiple times a day or you can’t keep down any fluids for more than 24 hours, you could get dangerously dehydrated.
Severe belly pain: Sharp, intense pain in your abdomen (especially upper abdomen) could mean pancreatitis. This isn’t the same as mild discomfort or bloating. It’s severe and might radiate to your back.
Signs of serious dehydration: Dark pee, dizziness when you stand up, racing heartbeat, barely peeing at all, extreme thirst you can’t quench, dry mouth, or confusion.
Vision problems: Any changes in your vision, blurriness, floaters, or trouble seeing needs immediate attention, especially if you have diabetes or diabetic eye problems.
Trouble breathing or swallowing: These could mean a severe allergic reaction or something else serious.
Severe allergic reaction: Difficulty breathing, bad rash, face or throat swelling, or other signs you’re having an allergic reaction.
Thoughts of hurting yourself: Some people experience mood changes on GLP-1s. If you have any thoughts of self-harm, get help immediately.
Call your doctor within a day for:
Symptoms that won’t improve: Nausea, fatigue, or other side effects that don’t get even a little better after 4-6 weeks, or that mess with your ability to eat, work, or live your life.
No bowel movement for 5+ days: Severe constipation that doesn’t budge with fiber, water, and walking, or that causes serious pain.
Losing weight too fast: Consistently losing more than 2-3 pounds a week might mean you’re not eating enough or your dose is too high.
New or worsening stuff: Any symptom that shows up after you’ve adjusted, or something that gets worse after it was getting better (and you didn’t increase your dose).
Can’t eat enough: If side effects stop you from getting adequate protein, calories, or essential nutrients for more than a few days.
Symptoms that come back: If you felt better and then symptoms return for no clear reason, something else might be going on.
You want to quit: If side effects make you want to stop the medication, talk to your doctor before you do. They might be able to lower your dose temporarily or prescribe something to help with symptoms.
Managing GLP-1 side effects is personal. What works amazing for your friend might not do much for you. Start with the basic strategies, be patient while your body adjusts, and speak up when you need medical help.
Most people feel way better within 4-6 weeks as their body gets used to the medication. Those rough first weeks are temporary. With the right approach and realistic expectations, you can handle the side effects while still reaching your weight loss goals.
And remember: you don’t have to just tough it out through awful symptoms. GLP-1 treatment should be tolerable. Work with your doctor to find the right dose and symptom management combo that lets you function normally while making progress.